Lighting the way
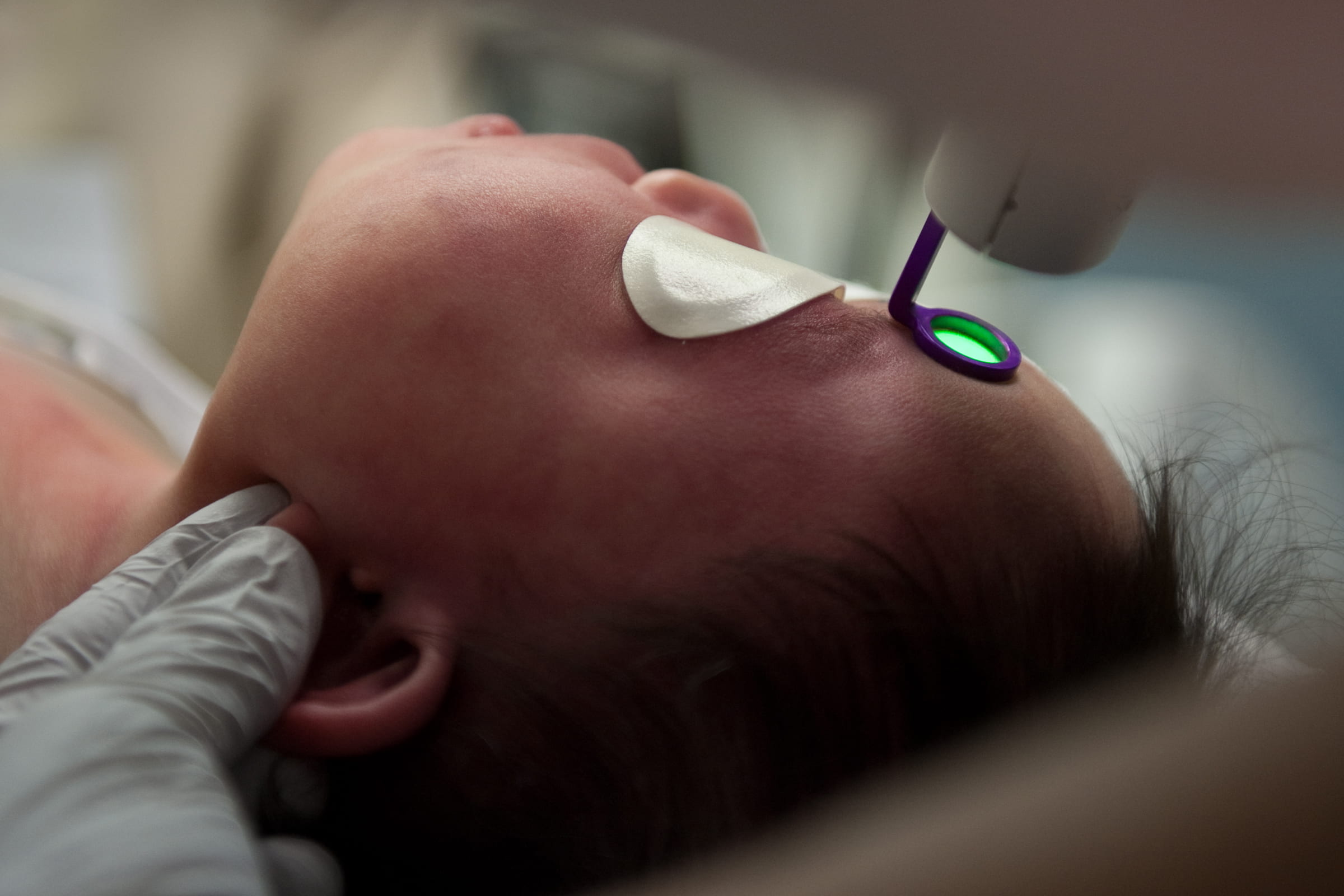
The concept that revolutionized laser surgery and earned UC Irvine more than $40 million came to Dr. J. Stuart Nelson in 1992 while he was watching a baseball game.
In the early 1990s, surgeons like Nelson were trying to adapt laser technology for medical use, and the Beckman Laser Institute & Medical Clinic was an epicenter for this effort. It was, at the time, the only facility in the world to house basic science and engineering labs and an outpatient clinic under one roof, letting researchers and surgeons quickly translate findings into patient-care breakthroughs.
As medical director of the BLIMC, Nelson had been striving to improve laser treatments for disfiguring vascular birthmarks, such as port-wine stains, in infants and young children. Laser’s utility was limited because its intense light also injured the fragile top layer of skin, causing pain, scarring and pigmentation changes. The challenge was to find a way to protect the outer skin while maximizing destruction of the deeper blood vessels that create a birthmark.
Nelson and his BLIMC colleagues – postdoctoral researcher Thomas Milner and visiting Norwegian engineer Lars Svaasand – had tried using ice cubes, running cold water and even the application of chilled metal plates to cool the skin’s superficial layer before laser exposure. Unfortunately, all of these methods proved too cumbersome and, more importantly, also cooled the targeted blood vessels, which inhibited the laser’s effectiveness.
“We needed to get something very cold onto the skin surface in perfect thermal contact and then off the skin surface – all within a fraction of a second,” Nelson says. “I remembered what I saw watching a baseball game.”
Over a Friday night dinner at the former Rusty Pelican restaurant in Irvine, he told his colleagues how, when a batter fouled a baseball off his foot or ankle, a trainer would emerge from the dugout and spray ethyl chloride onto the injury site to numb the pain. The three agreed that spray cooling might be effective with lasers if the cryogenic agent evaporated very quickly and, therefore, only affected the topmost layer of skin.
During the weekend, Milner and Svaasand hashed out ideas on how this concept could work; on Monday, they went to Pep Boys and purchased a Toyota Camry fuel injector valve, a hose clamp and air conditioning coolant to build the first prototype of the Dynamic Cooling Device.
To determine the optimal cryogen spurt duration and interval between spurt termination and laser exposure, all three researchers tested the DCD on themselves. “We still have scars on our arms to prove it,” Nelson says.
“It was a fairly simple construction,” says Milner, currently the Marion E. Forsman Centennial Professor in Engineering at the University of Texas at Austin. “That’s the beauty of the invention: It’s so simple and works so well.”
The device is incorporated into the laser’s hand piece and sprays a nonflammable, environmentally compatible freon substitute onto the skin surface, forming a liquid pool with a temperature of minus 60 degrees Celsius. This pool almost immediately evaporates, and milliseconds later, the skin is exposed to the laser. The process is repeated before each pulse of light.
“Because the spurt durations are so short, the cooling remains confined to the skin’s most superficial layer and does not affect the deeper targeted blood vessels causing the vascular birthmark,” Nelson explains. “This allows much higher laser light dosages to be used, while at the same time minimizing injury to the skin and pain to the patient.”
The DCD was patented in September 1998 and subsequently licensed to Candela Laser Corp. for commercial development and marketing. It’s now standard on more than 20,000 Candela lasers sold worldwide, as well as on the lasers of other companies that have sublicensed the technology.
Between 2001 and 2010, the device was among the 10 top-earning licensed inventions in the University of California system – and in 2005 and 2006, it ranked second and third, respectively. To date, the DCD has generated more than $40 million in royalties for UCI, of which almost $7 million has been returned to the BLIMC.
“The combination of basic research, engineering and clinical testing that went into the Dynamic Cooling Device is exactly what was envisioned over 30 years ago when the idea of the BLIMC was first conceived,” says Michael Berns, the Arnold & Mabel Beckman Chair in Laser Biomedicine and institute co-founder.
While DCD-equipped lasers are utilized for a number of cosmetic procedures – the removal of unwanted hair, scars and rosacea, for example – Nelson is pleased that his invention primarily benefits individuals born with port-wine stains. At the BLIMC’s world-renowned Vascular Birthmarks & Malformations Diagnostic & Treatment Center, he has handled more than 10,000 such cases.
Every other year, the BLIMC – in conjunction with the Vascular Birthmarks Foundation – hosts a conference at which families dealing with vascular birthmarks meet with researchers and surgeons in the field to discuss the latest findings and breakthroughs. This year’s conference will take place Nov. 4 and 5 at the Island Hotel in Newport Beach.
Nelson says events like these – where he interacts with new, current and former patients – remind him of the DCD’s impact.
“The technology has made possible the early, painless, safe and effective treatment of port-wine stains and other disfiguring vascular birthmarks in infants and young children in ways that Tom, Lars and I could never have imagined,” Nelson says. “That’s what I’m most proud of.”
Originally published in ZotZine Vol. 4, Iss. 2


