Finding OC’s true COVID-19 rates
UCI antibody study finds infection prevalence seven times higher than previously estimated

Even as official COVID-19 cases approach 9 million, researchers across the United States believe the actual numbers are higher, since people with few to no symptoms are rarely tested.
“There was this lurking suspicion that there’s a large fraction of people that have it that did not know,” says Tim Bruckner, an associate professor of public health at UCI. “Either they had symptoms and did not seek care, or they did not have symptoms and had no reason to go.”
Understanding how many people have had the disease helps identify at-risk groups, determines its true fatality rate and how easily the disease spreads, and gauges how far a community is from herd immunity. All of these factors assist in determining health guidelines and reopening the economy, as well as understanding the disease.

So UCI researchers, led by Bernadette Boden-Albala and Bruckner, teamed up with the Orange County Health Care Agency (HCA) to create the actOC study and find out the true prevalence of COVID-19 in Orange County.
They found that 11.5 percent of county residents have antibodies for COVID-19, which is seven times as many people as in previous estimates. Latinx and low-income residents had the highest prevalence rates at 17 percent and 15 percent respectively.
“The greater prevalence of a positive antibody response among Latinx populations is consistent with some of the testing and hospital data that has come out of Orange County and nationwide,” says Boden-Albala, director of UCI’s Program in Public Health and a co-principal investigator on the study. “As we look toward the fall and flu season, this data also justifies enhanced planning and resources in communities likely to be hit hardest.”
Testing Orange County
Working with marketing firm LRW Group, the UCI team enrolled more than 3,000 random participants that accurately represent the county’s diverse population. Using a UCI-developed imaging platform, they tested for a wide range of viral antibodies, distinguishing between SARS-CoV-2 and other coronaviruses such as SARS-CoV.
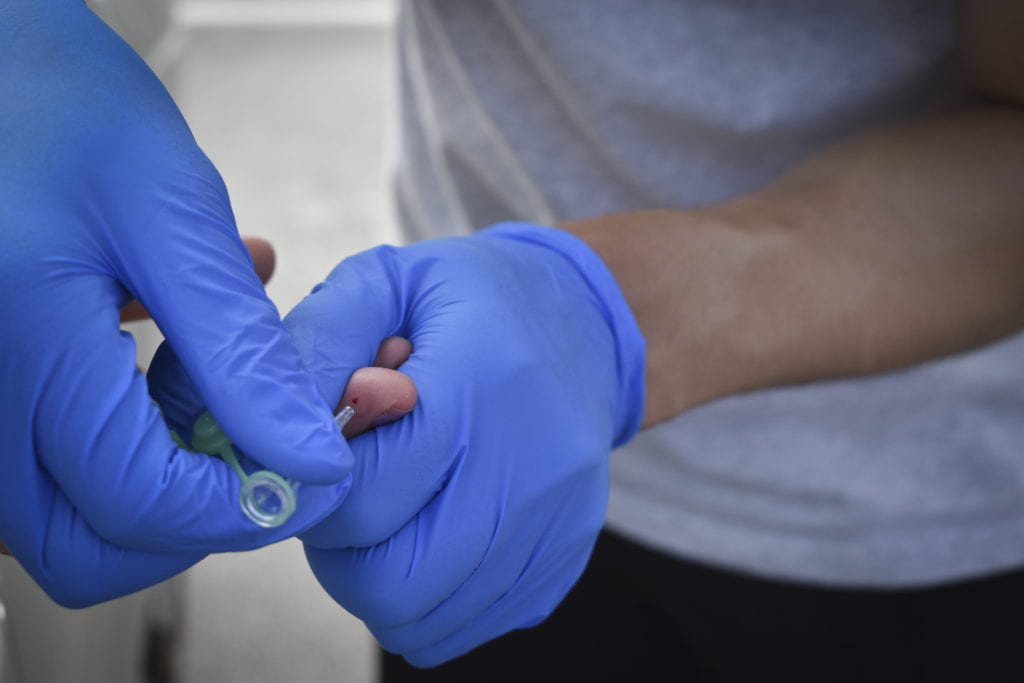
Carlos Puma for UCI Health
The researchers are following up with a subset of 200 people who tested positive. Every two weeks for four months, this group will be tested, so researchers can see how the immune response changes over time and what groups are most at-risk.
Participants visited one of 11 drive-through testing sites – selected based on HCA emergency plans – where medically trained volunteers collected blood samples using finger pinpricks. Most volunteers were UCI students and alumni.
“Not only was I able to help the community, I was able to get some hands-on experience working with the study participants which was extremely valuable,” says Joelle Ragland, a volunteer who received her bachelor’s in public health from UCI earlier this year. “I was able to get blood-borne pathogen certified and learn how to do the finger-pricks.”
A first for California
Recent surveys in other metropolitan regions of the U.S. also suggest that infection rates are higher and death rates lower than previously thought, and that rates vary significantly from place to place.
But this is the first study in California to use a sample that truly represents population diversity while testing for a wide array of viral antibodies, allowing for an accurate percentage of the disease’s prevalence in Orange County.
Separately from this study, UCI researchers plan to scale up production of the testing system to deploy across the U.S. by the end of the year. The low-cost, portable imaging platform could bring studies like this to low-resource areas in the U.S. and around the world.
It is not yet clear what level of antibodies indicates immunity for those who have had COVID-19, but continued follow-up with the people who tested positive will provide more information, as will similar projects globally. While 11.5 percent is still substantially below the minimum of 70 percent of residents required to achieve herd immunity – and while one county cannot act as a guide for the country as a whole – many researchers hope that representative antibody testing across the U.S. could help to guide reopening and public health decisions.
“Our study demonstrates that while a significant number of OC residents were already exposed and developed antibodies to COVID-19, much of the county still remains vulnerable,” says Boden-Albala. “There is a lot more work to be done.”



