In the wake of war
New UCI lecturer brings first-hand experience photographing Iraq to a new course on the public health effects of war.
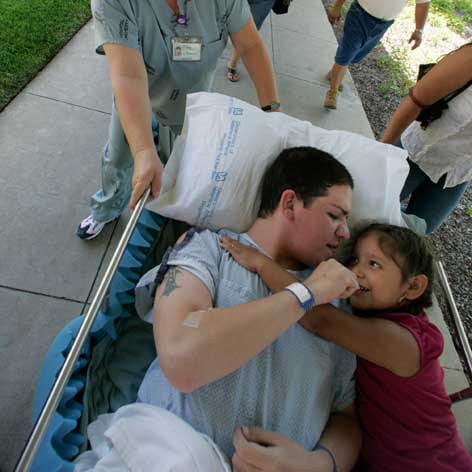
The last time Pauline Lubens saw U.S. Army Sgt. Frank Sandoval, she slapped the veins on her forearm and said, “If you need blood, I’m right here,” half-joking that if he needed a transfusion of their shared type of blood while undergoing surgery, she’d donate.
It was an unusually personal offer for a journalist, but she’d documented the soldier’s painful, liberating struggle back to health for a year. While Sandoval was on active duty in Iraq, shrapnel from an improvised explosive device had ripped into his brain. After months in a Palo Alto veterans hospital relearning how to walk and talk, he’d finally gone home to Yuma, Ariz. But now the husband and father of one needed to have a fairly routine flap put in his skull.
Sandoval, 27, never regained consciousness after the operation. His organs were donated, and he was buried with full military honors in Yuma.
The shattering event halfway through the Iraq War propelled Lubens, 56, into a new career as a lecturer in UC Irvine’s Program in Public Health. This winter for the second time she’ll teach a popular undergraduate course on the public health ramifications of war.
Those effects are numerous, Lubens says, particularly with modern wars like those in Iraq and Afghanistan. Multiple deployments, an all-volunteer army that means much of the public is not directly involved, families having women as well as men go to war and other factors will mean decades of mental and physical health woes for veterans.
The last of about 165,000 American military personnel returned from Iraq at year’s end, 32,000 of them wounded and as many as a third with serious mental health issues and possible brain damage, according to the Department of Defense and preliminary statistics. Lubens calls traumatic brain injuries like Sandoval’s “a signature wound of a signature weapon,” the improvised explosive device.
“I’ve never been interested in the bang-bang of wars. I’ve always been more interested in how the bang-bang affects soldiers and civilians,” Lubens says. She says those effects already have included spikes in domestic violence, post-traumatic stress disorder, and even car accidents.
Lubens explains that veterans who steered armored tanks overseas learned evasive driving techniques that are inappropriate on a crowded highway, and they may suffer from PTSD due to explosions and other attacks, causing them to overreact to traffic challenges.
While many experts say that bringing U.S. troops home will finally stop a $1 trillion budget hemorrhage, she argues that substantial funds must be set aside for their healthcare, including adequate money for veterans hospitals and other infrastructure.
Oladele Ogunseitan, chair of UCI’s fast-growing Program in Public Health, says Lubens is a good fit, citing her battlefield experience and degree from Johns Hopkins University’s Bloomberg School of Public Health: “We’re thrilled that Pauline joined us this fall quarter to share her award-winning work as a journalist in embattled areas and her training at one of the best public health academic institutions in the world. Her course was immediately oversubscribed.”
Lubens says she expected that some in her class would have family members fighting overseas, but there are not as many as she had thought. A significant number do, however, have parents who fled war-torn Cambodia, Vietnam, Afghanistan and other Middle East hot spots.
That dovetails with one of her major research interests: the re-traumatization of refugees in the U.S. Often, for instance, they can only find housing in crime-ridden neighborhoods like one she studied in Baltimore.
“My two passions are the military community and the Iraqi refugee community, but these are not always communities
that see eye to eye,” Lubens says. “I meet with both, and they’re such different conversations.”
She’s thrilled with her career switch, feeling that her work now has real meaning.
“It’s amazing; I feel completely rejuvenated,” Lubens says. “Am I nervous about how I’m going to make a living? Yes. But I love, love, love teaching.”