Blocking inflammation prevents cell death, improves memory in Alzheimer’s disease
UCI mouse study points to new treatments to limit effects of neurological disorder
Irvine, Calif., Feb. 29, 2016 — Using a drug compound created to treat cancer, University of California, Irvine neurobiologists have disarmed the brain’s response to the distinctive beta-amyloid plaques that are the hallmark of Alzheimer’s disease.
Kim Green and colleagues with UCI’s Institute for Memory Impairments and Neurological Disorders found that flushing away the abundant inflammatory cells produced in reaction to beta-amyloid plaques restored memory function in test mice. Their study showed that these cells, called microglia, contribute to the neuronal and memory deficits seen in this neurodegenerative disease. Results appear online in the journal Brain.
“Our findings demonstrate the critical role that inflammation plays in Alzheimer’s-related memory and cognitive losses,” said Green, an assistant professor of neurobiology & behavior. “While we were successful in removing the elevated microglia resulting from beta-amyloid, further research is required to better understand the link among beta-amyloid, inflammation and neurodegeneration in Alzheimer’s.”
The neurobiologists treated Alzheimer’s disease model mice with a small-molecule inhibitor compound called pexidartinib, or PLX3397, which is currently being used in several phase 2 oncology studies and a phase 3 clinical trial to treat a benign neoplasm of the joints.
The inhibitor works by selectively blocking signaling of microglial surface receptors, known as colony-stimulating factor 1 receptors, which are necessary for microglial survival and proliferation in response to various stimuli, including beta-amyloid. This led to a dramatic reduction of these inflammatory cells, allowing for analysis of their role in Alzheimer’s. The researchers noted a lack of neuron death and improved memory and cognition in the pexidartinib-treated mice, along with renewed growth of dendritic spines that enable brain neurons to communicate.
Green said that although the compound swept away microglia, the beta-amyloid remained, raising new questions about the part these plaques play in Alzheimer’s neurodegenerative process.
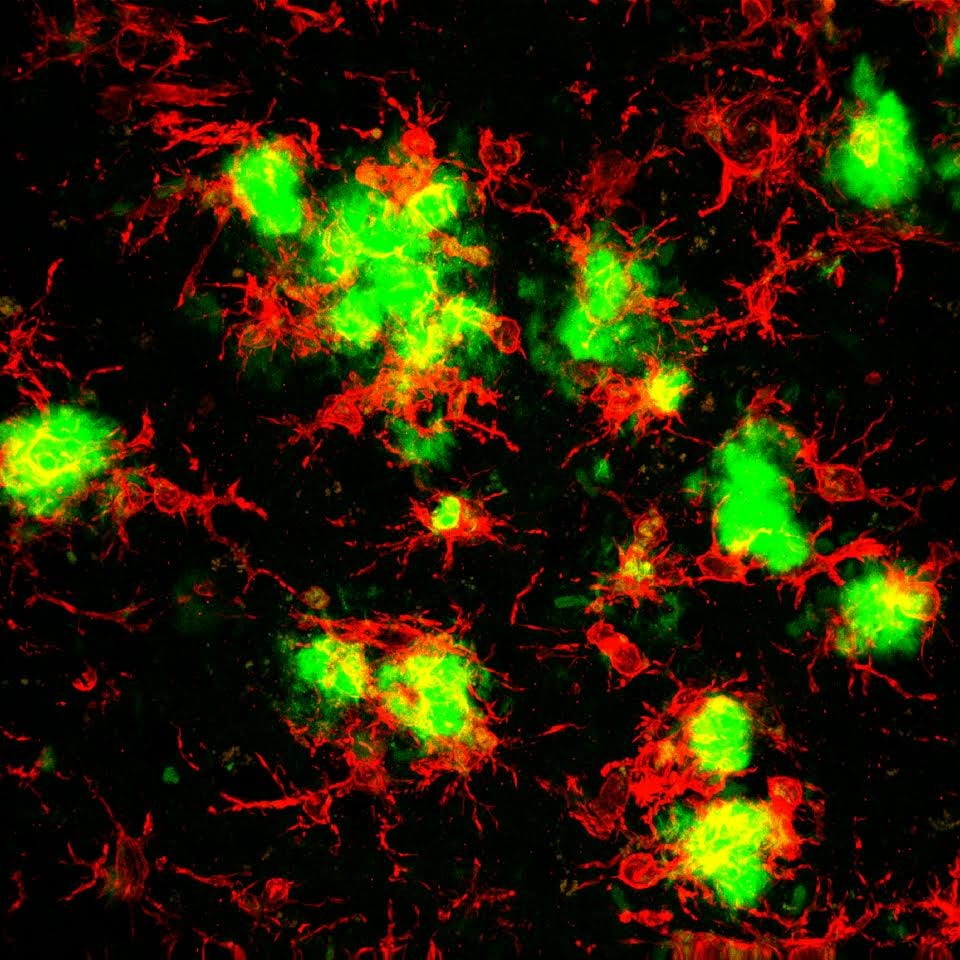
In healthy tissue, microglia act as the first and main form of immune defense in the central nervous system. But in a disease state, such as Alzheimer’s, microglia appear to turn against the healthy tissue they were originally assigned to protect, causing inflammation in the brain. The beta-amyloid plaques in brain areas related to Alzheimer’s disease are rich with these rogue microglia, Green added.
“Our work is telling us that these cells may contribute to the disease process, and targeting them with such specific drugs is a promising new approach,” he said.
Elizabeth Spangenberg, Rafael Lee, Allison Najafi, Rachel Rice, Monica Elmore and Mathew Blurton-Jones of UCI and Brian West of Plexxikon Inc. contributed to the study, which was supported by the National Institutes of Health (grants 1R01NS0833801 and P50AG016573), the Whitehall Foundation, the American Federation for Aging Research and the Alzheimer’s Association. Plexxikon Inc. provided the pexidartinib compounds.
About the University of California, Irvine: Currently celebrating its 50th anniversary, UCI is the youngest member of the prestigious Association of American Universities. The campus has produced three Nobel laureates and is known for its academic achievement, premier research, innovation and anteater mascot. Led by Chancellor Howard Gillman, UCI has more than 30,000 students and offers 192 degree programs. It’s located in one of the world’s safest and most economically vibrant communities and is Orange County’s second-largest employer, contributing $4.8 billion annually to the local economy. For more on UCI, visit www.uci.edu.
Media access: Radio programs/stations may, for a fee, use an on-campus ISDN line to interview UC Irvine faculty and experts, subject to availability and university approval. For more UC Irvine news, visit wp.communications.uci.edu. Additional resources for journalists may be found at communications.uci.edu/for-journalists.