Ultrasound in the ER: Wave of the future
Portable ultrasound scanners in the ER can save lives by expediting diagnosis.
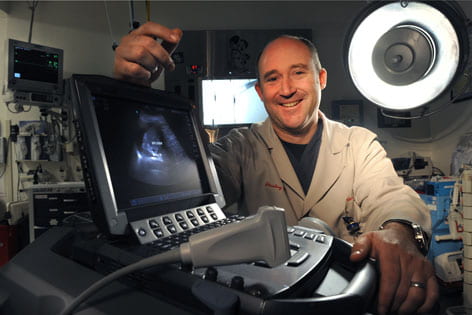
All too often, a stethoscope and a doctor’s touch are still the primary tools for diagnosing emergency-room patients. UC Irvine physician Chris Fox aims to change that.
Rather than feeling for a broken bone or swollen abdomen or merely listening to the heart, Fox has trained UC Irvine Medical Center’s emergency department clinicians to use the latest in lightweight, high-resolution ultrasound scanners, allowing them to diagnose in minutes — and with striking precision — life-threatening conditions requiring immediate intervention.
The emergency-medicine doctor became an evangelist for ultrasound when a young woman with breathing problems was rushed to the Chicago hospital where he was learning to use the device. She seemed to be having an asthma attack, but her lungs were clear, so Fox moved the sound-wave probe lower and saw that her abdomen had filled with blood, which he quickly traced to a fetus developing outside her uterus. She was rushed into surgery.
“Without the ultrasound scanner, she would have died from a ruptured ectopic pregnancy,” says Fox, co-author and editor of Clinical Emergency Radiology, a new textbook on the use of ultrasound in the ER. “We knew immediately what we needed to do.”
Ultrasound has long been a staple of obstetrics. The technology has developed rapidly in recent years, allowing cardiologists, urologists and others to peer inside the body with a clarity that makes minimally invasive surgical techniques, such as heart catheterization and clot removal, safer and more effective. Some scanners, which work by emitting sound waves to plot images on a computer screen, can produce three-dimensional results.
With portable devices that weigh less than 7 pounds, fire up in 15 seconds and cost about $50,000, trained clinicians can identify 44 medical conditions with a high degree of accuracy in two minutes. They can detect collapsed lungs, gallstones, blood clots, heart problems and blockages in the stomach, intestines and kidneys.
When a 40-year-old car crash victim was wheeled into UC Irvine’s emergency room recently, his pulse stopped, suggesting heart failure. But by moving the ultrasound probe over the man’s chest, Fox saw that blood had flooded the sac surrounding his heart, constricting its ability to pump.
“We cracked his chest open right there and found the cause of the bleeding, which was a hole in the right ventricle,” Fox says. “We temporarily closed it, stabilized the patient for more definitive care in the operating room — and he survived.”
The scans minimize “the shotgun approach we have had to take in emergency medicine,” says Fox, UC Irvine’s director of emergency ultrasound and an associate clinical professor who has written 20 peer-reviewed articles and an earlier textbook on the subject.
“We now have the ability to look through the skin, right at the organs we’re interested in,” he adds. “We can see tears in tissue, in muscles and tendons. Not since the stethoscope have we been able to find out what’s going on inside the body without something more invasive, like X-rays. With ultrasound, there’s no radiation, just sound waves.”
U.S. military medics already have battery-operated ultrasound machines on the battlefield. NASA astronauts have them on the space shuttle. And researchers at remote Antarctic stations are being trained to use them.
Yet only a few hospital emergency rooms in Orange County — indeed, in Southern California — use ultrasound for diagnosis, Fox says.
He credits UC Irvine’s director of emergency medicine, Dr. Mark Langdorf, with the foresight to send him almost a decade ago to the Chicago ultrasound program, where Fox became the nation’s third ER physician to specialize in emergency radiology. Today there are 44 emergency radiology fellowship programs, including UC Irvine’s.
When not in the ER or teaching, Fox is spreading the word about diagnostic ultrasound. He has given lectures in seven countries, 47 states and throughout Southern California
Fox won’t be satisfied until ambulances carry ultrasound scanners. “The next step,” he says, “is to push this equipment out into the field, with the paramedics, pre-hospital.”